Oversight That Matters: Lessons for Boards
This article shows why most SMB healthcare organizations get quality wrong. It distinguishes QA (process compliance) from QI (performance improvement), highlights regulatory requirements like Medicare/Medicaid QAPI, and explains the real impact on finances, operations, and Board oversight.
RISKBOARD OF DIRECTORSQUALITY AND IMPROVEMENT
Richard A. Raphael
3/18/20262 min read

Disclaimer: The views expressed in this article are my personal opinions and do not reflect the views or policies of any affiliated organization. This article is intended for informational purposes only and should not be construed as anything else.
Most small- and mid-sized businesses (SMB) in healthcare are compliant—but not improving. They fail to distinguish between Quality Assurance (QA) and Quality Improvement (QI), using the terms interchangeably or building fragmented processes. The result: compliance gaps on one end, stagnation on the other.
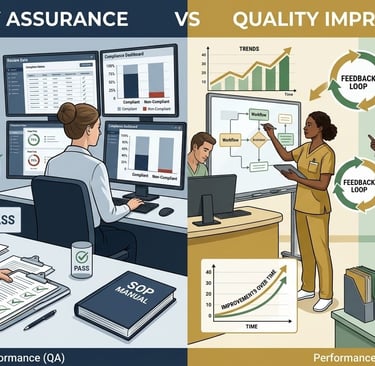
At its core: QA is about conformance. QI is about performance. Most SMB are doing a weak version of one—and calling it both.
In practice, “quality” often shows up as periodic chart audits, basic checklists, reactive issue tracking, and disconnected metrics. That’s not a quality system—it’s scattered activity. What’s missing are two distinct but connected frameworks: a QA framework to ensure standards are met, and a QI framework to drive measurable improvement over time. Without both, organizations drift out of compliance or plateau operationally.
A real QA framework includes process standardization, structured documentation, inspection and validation, compliance metrics, staff training, and governance aligned with regulatory and contractual requirements. QA answers: are we doing things the way they’re supposed to be done? It is static and protective—it locks in a standard and enforces it.
QI, by contrast, focuses on outcomes, trends, root cause analysis, process redesign, feedback loops, and cross-functional collaboration. It answers: are we getting the best possible results—and how do we improve them? QI is dynamic, forward-moving, and challenges the standard rather than protecting it.
Most SMB default to light QA and assume that’s enough. They audit charts, fix documentation issues, and pass inspections and accreditation surveys—but denial rates remain high, throughput lags, inefficiencies persist, and margins stagnate. For example, average claim denial rates in U.S. healthcare cluster around 10–15%, with many providers reporting 10% or higher on initial submission. Organizations that adopt structured QI approaches—analyzing trends, addressing root causes, and redesigning workflows—have documented reductions to 4–6% within months (Azebra Tech, 2023). QA alone cannot achieve this improvement; it only verifies existing processes.
Healthcare contracts and regulations are structured around QI, not just QA. Medicare Advantage plans require ongoing quality improvement programs with measurable outcomes. Medicaid managed care mandates formal QI programs and performance improvement projects. CMS Conditions of Participation require providers to implement Quality Assessment and Performance Improvement (QAPI) programs. Value-based care, star ratings, and incentive payments all depend on continuous improvement, not static compliance.
Boards in SMB healthcare feel this directly. The impact consolidates into three critical areas:
Governance & Regulatory Oversight – Boards have a fiduciary duty to oversee both compliance and performance. Weak QA or absent QI creates blind spots in risk and regulatory management, especially under Medicare and Medicaid requirements.
Financial & Strategic Impact – QI drives reimbursement, operational efficiency, and margin. Without it, the Board sees stagnant or declining performance, approves strategies the organization cannot execute, and limits growth.
Data & Reporting Integrity – QA-driven dashboards give a false sense of control. Boards need trend analysis, root cause visibility, and evidence of sustained improvement to make informed decisions.
If QA protects the floor and QI raises the ceiling, the Board is accountable for both. Without properly structured QA and QI, Boards aren’t just overseeing weak quality systems—they are operating without real visibility into risk, performance, or strategic execution. In healthcare, that gap compounds quickly and has real regulatory, operational, and financial consequences.
Souture
Contact Us:
18 Maple Avenue, #164
Barrington, Rhode Island 02806
info@souture.io
